A Caregiver Companion
What is it?
The Caregiver Companion is a tool to support caregivers of cancer patients who have received a bone marrow transplant in the outpatient setting. It is a digital application that encapsulates and emulates a service instead of merely delivering education in a library format. The intent is to prepare caregivers before the process and support them throughout the process, connecting them to community, supporting symptom assessment, education, and pragmatic considerations throughout a very stressful journey.
With Dr. Lauren Bangerter | Mayo Clinic | Robert D. and Patricia E. Kern Center for the Science of Healthcare Delivery | Timeline: 3 months
My Role
Project Lead | Exploratory Research Synthesis | Journey Mapping | Insight Generation | Concept Development | Workshop Facilitation | Grant Writing | UX Design | Wireframing | Content Strategy | Information Architecture
Understanding the Problem
Bone marrow transplant (BMT) is one of the most stressful, costly, and intensive cancer treatments used to treat multiple hematologic malignancies and some solid tumors. BMT is one of several treatments that has gravitated from the inpatient to the outpatient setting, and with this shift, care responsibilities are now placed chiefly on family caregivers who, in addition to taking significant precautions to help patients avoid infection, must strictly monitor side effects, compliance to medication, diet, and activity. The potential strain on caregivers is tremendous as they provide support throughout transplant, and for months to years post-transplant.
Starting with Data
A qualitative analyst had already completed initial exploratory interviews with 10 stem cell transplant recipient caregivers, so to develop an understanding of the end users, I read all transcripts two times before I started any analysis. While the notion of developing empathy from transcriptions seems counterintuitive, because they were transcribed verbatim, it was easy to understand the caregivers’ lived experiences.
An Analysis Framework
Creating an analysis framework using a journey map as inspiration, as well as defined stages of the journey, allowed us to capture positive experiences, negative experiences, and quotes that we eventually used to affinitize and develop a final journey map.
Synthesis
Beginning synthesis with individual patient journeys within the above framework made the final synthesis less overwhelming, and allowed us to systematically record quotes, thoughts, and feelings to identify patterns that helped us create a more generalizable journey.
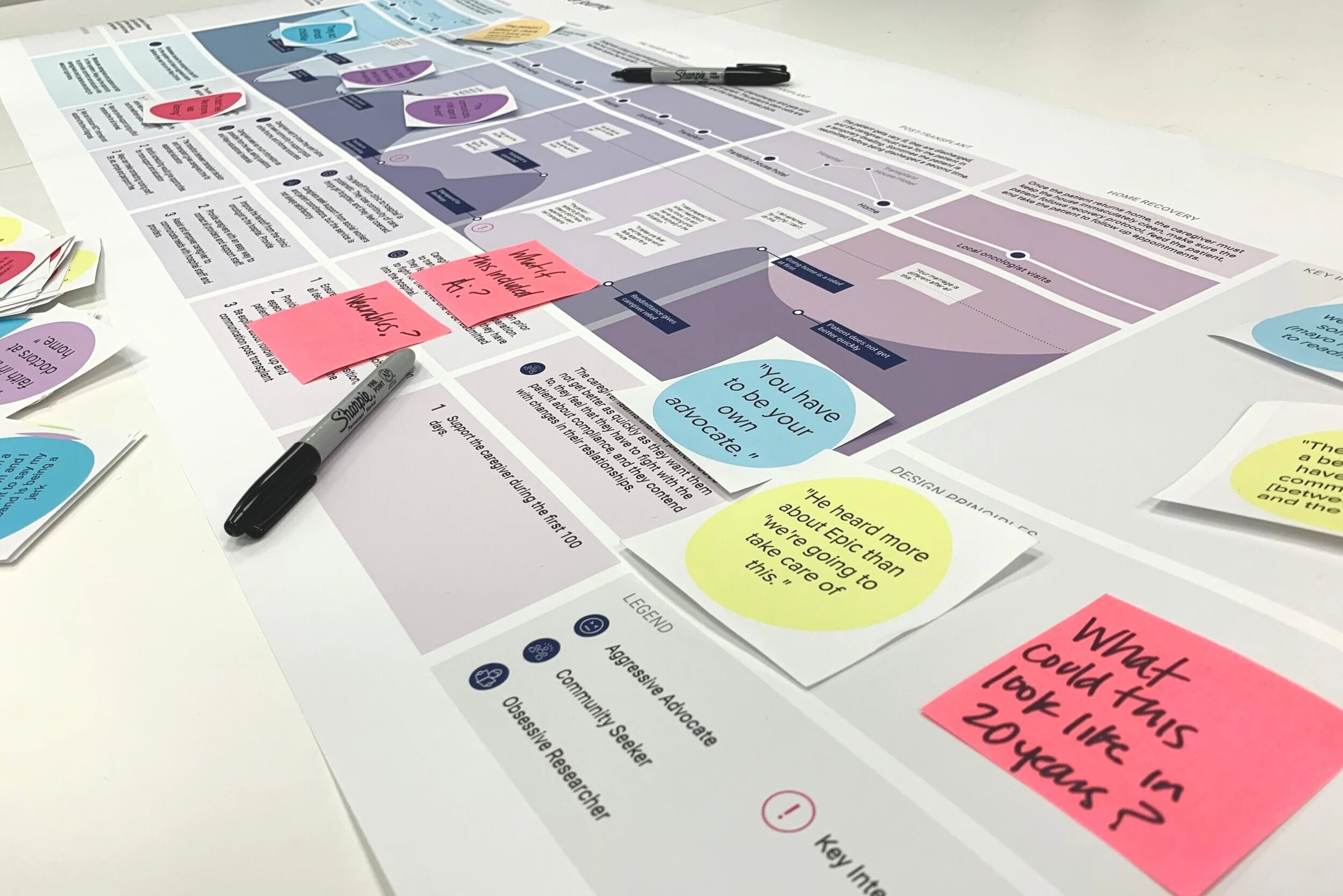
A Journey Map
After several hours of controlled chaos, we created a journey map to help the interdisciplinary team easily understand the caregiver experience and the associated low points and opportunities for improvement.
Insights and Opportunities
Transitional periods are stressful for caregivers
Periods of transition spatially, temporally, and emotionally are difficult for all involved in a cancer diagnosis and BMT treatment plan; however, there is an opportunity to improve these low-points with a well-designed intervention that removes friction from the experience.
Information about the transplant is not sufficient
The current state of education is a deluge of information given at one time, but it focuses primarily on disease progression, side effects, and other medically related information. Unfortunately, information for the caregiver to have an easier experience (i.e. how to talk to the patient), is notably absent.
Community is everything
Most caregivers want access to community and support, but the current state of HSCT creates a disparity between those with access to community and those who feel isolated. There is an opportunity to make sure all caregivers can connect with caregivers around them in a meaningful way.
Symptom assessment in the outpatient setting is stressful
The outpatient period directly after discharge is stressful for the caregiver because the responsibility of medical care is put on them, with little training, and there is a lot of fear associated with life-threatening complications, should they arise.
Concept development
In order to develop solutions and ideas for our identified opportunities, as well as help teach our research colleagues about the value of design, we held two brainstorming workshops to help be as divergent as possible.
Workshop Methodology
The workshop was comprised of cognitive psychologists, sociologists, healthcare services researchers, and other designers. We used the journey map as a framework to talk about opportunity areas, and used quote cards from the interviews to inspire discussion about what could be changed. Finally, we developed a list of emerging technologies and future trends to create a flexible brainstorming equation.
Synthesis
Future State Concepts
From the brainstorming workshop, we created seven future state concept vignettes including future and emerging technologies, service concepts, application ideas, and other types of interactions to improve the future of bone marrow transplant caregiver journeys.







Concept & Content Evaluation
Methodology
We conducted 5 evaluative sessions with bone marrow transplant caregivers to elicit freeform narratives of their experiences, speed dating exercises, where users evaluated future state concepts, and a content card sort to understand what types of information would be most valuable at different stages of the caregiver journey.
Concept Insights
While initial journey mapping and synthesis revealed themes and initial solutions, the scenario evaluation revealed deeper needs, refuted some of our hypotheses, and supported some of them. We distilled the findings into actionable insights to apply to the application design.
Discomfort with Emerging Technology
Caregivers did not respond positively to the idea of using a wearable or other sensors to monitor the patient’s vital signs and temperature, indicating that they wouldn’t trust that it was correct. Instead, they were more likely to use a regular thermometer and manually keep track of values.
Caregiver Wellness Suggestions Were Superfluous
Participants indicated that suggestions such as doing yoga, going to the gym, and depression check-ins would have been both superfluous and even “annoying.” Many caregivers indicated that they were so focused on the health of their patients that they were not concerned with themselves.
New Types of Content Are Useful
Our hypothesis was that adding extra value to the application would manifest in new types of content, such as strategies for coping with with the healthcare system, relationship changes, pragmatic lists, and stories from other caregivers were well-received and perceived as useful.
Future Service and Workflow Support Will Make the Intervention Stronger
Because caregivers have different experiences with symptom severity, technology in general, and the healthcare system, touchpoints with social workers or RNs in concert with the application should also be designed to ensure engagement and to understand when situations might require a person instead of a digital intervention (i.e. very severe symptoms).
Preparation Now and Being Able to See the Future is Vital
Caregivers want flexibility in their access to education; all participants want access to everything at the beginning, but also want to be guided through the process to prevent being overwhelmed during the transplant journey.
Content Strategy +
Information Architecture
Methodology
We used a card sort activity that allowed users to place different types of content, including educational materials, support materials, and pragmatic information across the different phases of the bone marrow transplant journey.
Results
Results suggest that the pieces of information with the highest frequency (4-5 participants) are more universally favored than content that only garnered attention from 1-2 participants. While the least favored content should not be omitted from the application, it suggests that there are both universal and personalized needs to address.
Total Frequency
Pre-Transplant Prep vs. Throughout the Experience
Participants placed 28 individual pieces of information in the “throughout” category and in the “pre-transplant prep” category. However, both categories suggest that caregivers want information and education available early and often so that they can feel prepared throughout their journeys.
Pre-transplant Prep
Throughout the Experience
Insight
When content is sorted into overarching themes, such as symptoms, social support, and transparency, it tells a lucid tale about what types of content would be most useful to the most people, as well as what types of content might be most useful in a personalized setting.
High Priority Content for Everyone
Social support
Symptom education
Recovery information
Contact Information
Understanding the process (advocacy, hospital, coordination, etc.)
Logistical information and equipment list (this was suggested to us by all participants, but not included in our card sort
Personalized Content
Information about moving to Rochester (not everyone moves)
Hotel information
Restaurants in the city
How-to videos
Information for a specific type of cancer; i.e. Multiple Myeloma vs. Lymphoma
Designing the Application
Early Sketches
Key Features
Concept and content insights from the evaluation phase allowed us to distill the application into useful features, informed the information architecture, and helped us create typologies of content to be developed as the product matures.
Guided Process
Because different types of information are needed at different points in time, a timeline with suggestions for activities, preparation, and education allows the caregiver to see what is ahead while also directing them to useful information at the right time. Further, the timeline was designed to feel personalized based on our research and knowledge of the journey, but it is simple and technically feasible, which is important for a grant funded study.
Personalization
Although a user profile has not been developed at this time, the real application will allow the user to enter information, such as the Mayo Location, the type of cancer being treated, and other needs. This will avoid presenting content that is not relevant to the user’s context.
Symptom Management and Assessment
One of the most significant pain points caregivers experience is anxiety surrounding assessing symptoms. This feature was developed to help the caregiver see progress from one week to the next, explain symptoms to physicians and health staff, as well as alert the caregiver when a symptom is dangerous and nudge them to call the nurse’s station.
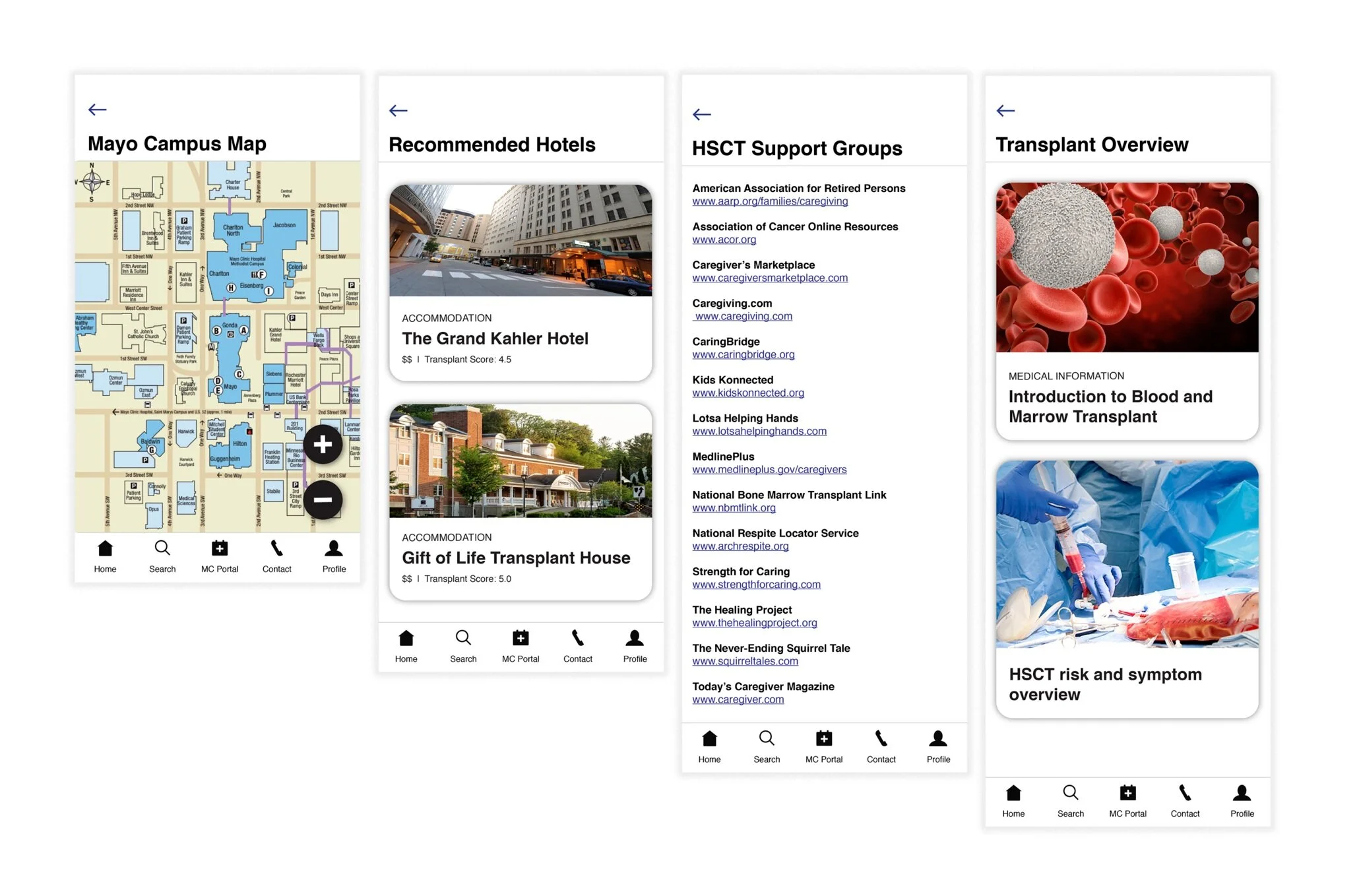
Practical Information
All participants indicated a need for pragmatic information to include items to purchase ahead of time to prevent going to the drug store at midnight for a new thermometer. Hotels and how-to videos were also missing from current state information.
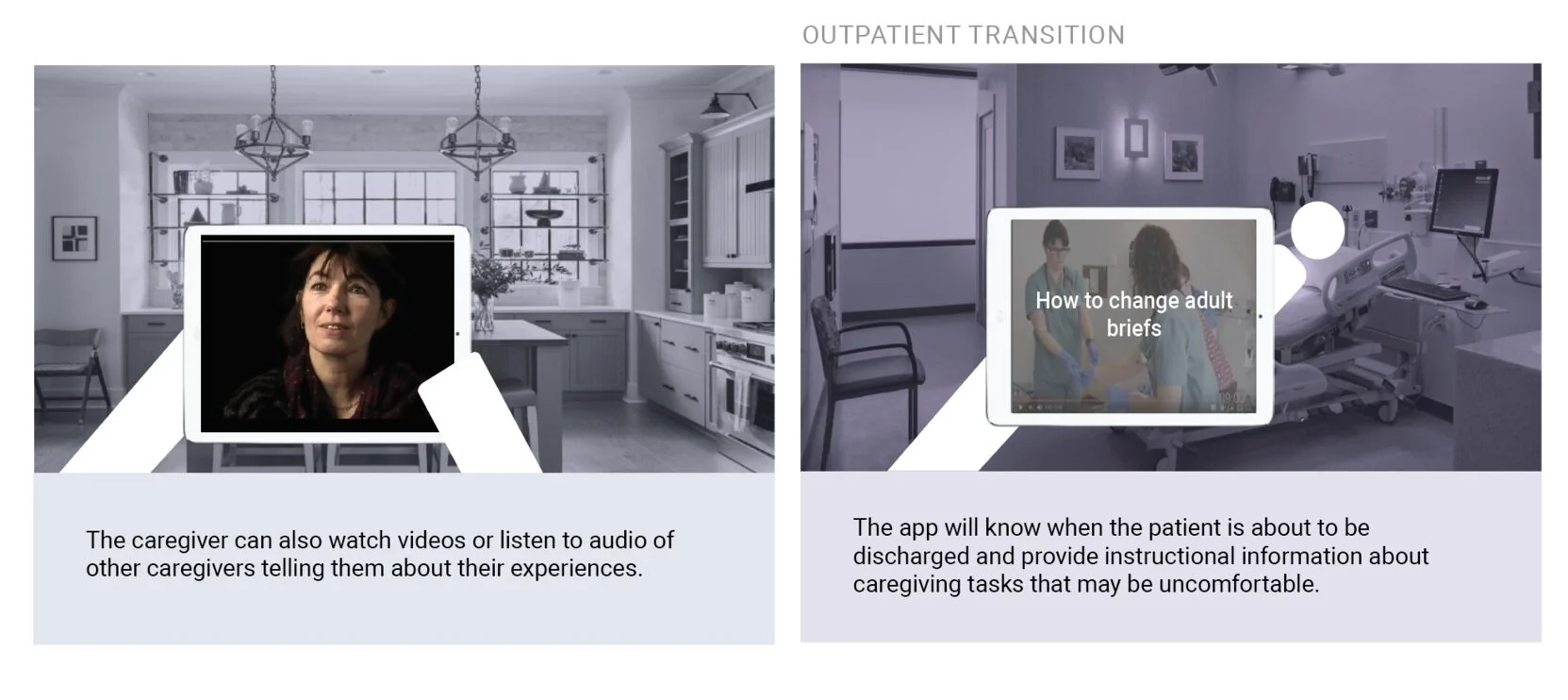
Handoff to Secondary Caregivers
During recovery from the bone marrow transplant, caregivers are required to be available to the patient 24 hours a day. Because this is not always possible, several caregivers had “secondary caregivers” to fill in when they could not. We wanted to create an easy way to share vetted educational materials with these users as well.
Finding Community
By and large, finding community was the most important aspect of the caregiver experience, so we created a feature that allows the caregiver to contact other caregivers in the area, creating an organic support network during the journey.
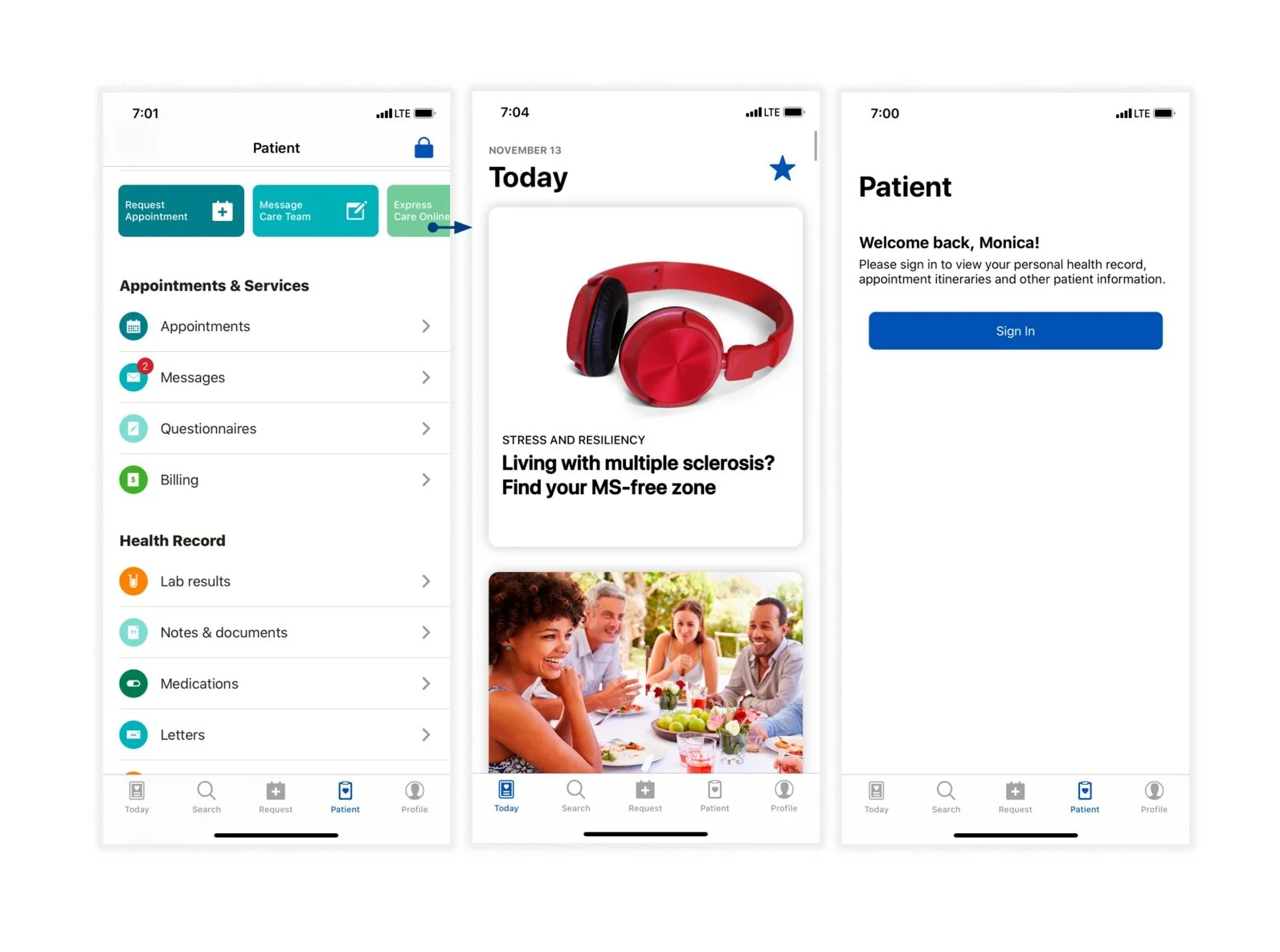
Visual Language
Keeping it in the Family
The visual design chosen for the application follows the Mayo Clinic Design System, which is the same as what patients see on the Mayo Clinic mobile portal. We believe that keeping the experience consistent across the Mayo Clinic is important for user trust and orientation, especially when users of this application are, on average, over 60 years old.
Impact
“You completely changed the way I look at my research; it’s more interesting, creative, and successful. I learned so much from you.”
The project’s impact at the Mayo Clinic and throughout the Center for Innovation was fourfold: a successful collaborative project with a truly multidisciplinary team, including designers, cognitive psychologists, sociologists, quantitative analysts, physicians, caregivers, and patients created a model for transformative projects across the Mayo Clinic. The project also created an entirely new paradigm for the intersection between implementation science, intervention studies, and design. We learned that design has the ability to result in a more successful research study, prevent wasted time due to poorly designed interventions, and more importantly, grant money. Finally, submission of this phase of research resulted in another $50,000 grant to fund usability testing, refinement, and a pilot study, which is currently in flight. The project was also awarded an $800,000 grant from the American Cancer Society and is currently under review for publication.
Looking to the Future
While the application is still in prototype phase, we have begun user testing with caregivers who previously participated in concept development. We’re already learning about the imperfections of the design, plan to iterate, refine, and do one more round of testing before shipping the product and conducting a randomized control trial to measure the impact in practice.